The True Cost of Manual Referral Processing
Manual fax processing costs DME providers far more than they realize. We break down the real numbers, from per-referral costs to annual losses for a 20-location operation.
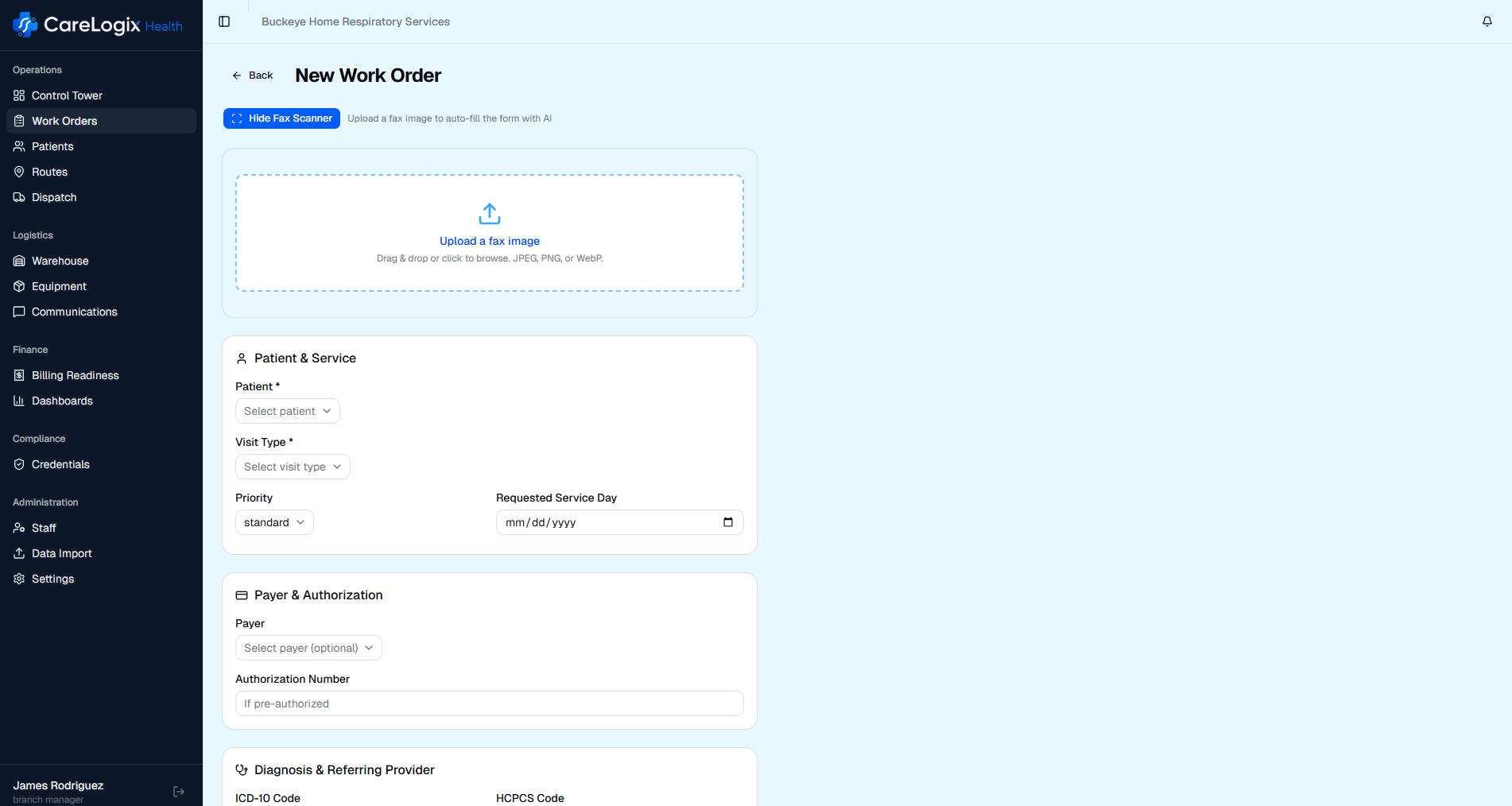
Every DME provider knows the routine. A fax arrives, someone pulls it off the machine (or out of a digital queue), squints at the handwriting, and starts keying data into the system. It takes somewhere between 8 and 12 minutes per referral, depending on legibility, missing fields, and how many times the intake coordinator has to pick up the phone to clarify something. Most operators accept this as the cost of doing business. But when you actually run the numbers, the true cost is staggering.
The Per-Referral Math
Let's start with time. An experienced intake coordinator processing a standard referral fax spends an average of 10 minutes on data entry alone. That includes reading the document, identifying the patient and physician, matching the order to HCPCS codes, verifying insurance information, and entering it all into the system. But that 10 minutes doesn't account for the follow-up work: calling the physician's office for missing signatures, chasing down incomplete face-to-face documentation, or re-entering data after a keying error.
When you include those downstream tasks, the real time investment per referral climbs to 15-20 minutes. At an average fully loaded labor cost of $22 per hour for intake staff, that's $5.50 to $7.30 per referral just in direct labor. For a provider processing 200 referrals per day across 20 locations, that adds up to $1,100 to $1,460 in daily labor cost for intake alone.
The Error Tax
Manual data entry error rates in healthcare hover between 2% and 5%. In DME referral processing, where staff are reading faxed handwriting under time pressure, real-world error rates are often closer to the high end. Each error has a cascading cost. A miskeyed insurance ID means a claim denial. A wrong HCPCS code means a rework cycle. A misspelled patient name means a failed eligibility check.
Conservative estimates put the cost of correcting a single data entry error at $25 to $50 when you factor in staff time, resubmission delays, and potential write-offs. At a 4% error rate on 200 daily referrals, that's 8 errors per day, costing $200 to $400. Over a year, error correction alone costs $52,000 to $104,000.
The Delay Cost
What's harder to quantify, but arguably more damaging, is the cost of delay. When referrals sit in a queue waiting for manual processing, patients wait longer for their equipment. In respiratory care, a 24-hour delay in getting a patient their CPAP or oxygen concentrator isn't just an inconvenience. It's a clinical risk and a satisfaction issue that affects referral relationships.
Physicians notice when their patients call back asking where their equipment is. Over time, slow turnaround erodes referral volume. If manual processing delays cost you even 5% of referral volume through physician dissatisfaction, a provider doing $10 million in annual revenue is leaving $500,000 on the table.
The Annual Picture for a 20-Location Provider
- Direct labor for intake: $286,000 to $380,000 per year
- Error correction costs: $52,000 to $104,000 per year
- Lost referral revenue: Potentially $250,000 to $500,000 per year
- Staff turnover: Intake roles have some of the highest burnout rates in DME operations, adding $15,000 to $20,000 per replacement in recruiting and training
All in, the true annual cost of manual referral processing for a 20-location provider easily exceeds $600,000, and often approaches $1 million when indirect costs are included.
How Automation Changes the Math
AI-powered referral intake doesn't eliminate human oversight. It eliminates the manual bottleneck. When a fax arrives and is automatically parsed, validated, and entered into the system in under 60 seconds, your intake coordinators shift from data entry clerks to exception handlers. They review flagged items, manage complex cases, and maintain physician relationships instead of squinting at handwriting.
The result is a dramatic reduction in per-referral cost, error rates that drop below 1%, and turnaround times that make physicians prefer sending referrals to you over the competition. The math isn't theoretical. It's the difference between growing and standing still.
The providers who thrive in the next five years won't be the ones who process faxes faster. They'll be the ones who automated intake entirely and redeployed their people to higher-value work.
About the Author

Adam Donaldson
Founder, CareLogix Health
Adam built CareLogix after years of implementing field operations systems at enterprise DME providers. He saw firsthand how fragmented tools, manual processes, and disconnected workflows cost branches hours every day and leak revenue that should have been captured. CareLogix is the platform he wished existed when he was on the implementation side.
Connect on LinkedInSee CareLogix in Action
Schedule a 30-minute walkthrough and see how CareLogix manages the full work order lifecycle for DME providers like you.